Blood Transfusion In Animals
Introduction
As in humans, blood transfusion in animals can be a life saving procedure. It is done in the following conditions:
Hemorrhage
- When hemocrit (HCT: Volume of RBCs per 100 ml of blood) has fallen below 20% in dogs and 15% in cats
- Deficiency of blood constituents
- Autoimmune hemolytic anemia
- Surgery
- Abomasal ulcer
- Anaplasmosis (a tickborne disease of RBCs)
- Theleriosis (a tickborne disease of lymphocytes)
- Babesiosis (a tickborne disease affections RBCs)
Pallor, tachycardia (rapid heartbeat), tachypnea (abnormally rapid breathing), snappy or thread pulsed, and decreasing mental activity are immediate signs that the patient likely needs a blood transfusion.
However, transfusion increases the risk of infection, blood transfused diseases and immune reactions and hence, as a general rule, if an effective alternative is available, should be avoided.
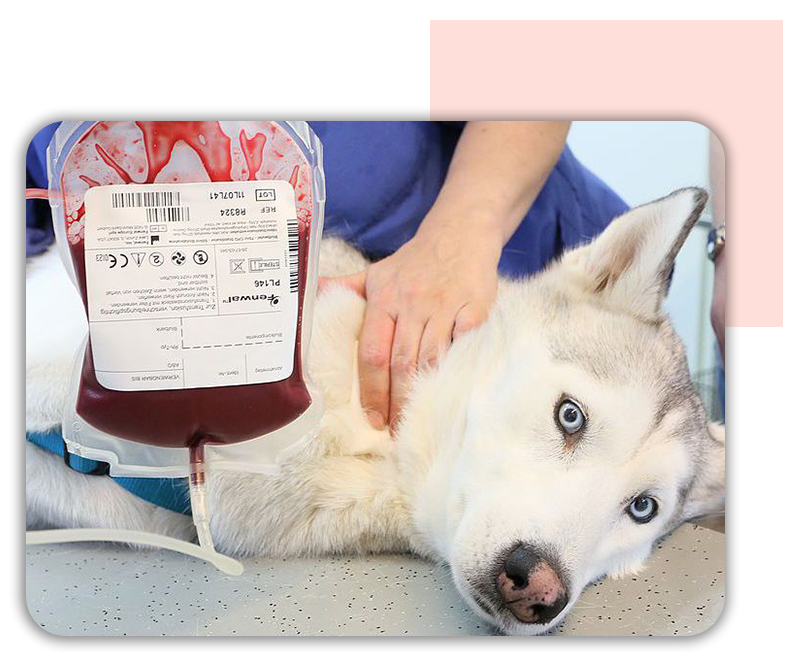
Blood Typing/Cross Matching
Before transfusing, patients should ideally undergo blood typing and tests depending on previous transfusions, history of pregnancy, etc. to predict and detect any future complications like the risk of any transfusion diseases.
Blood groups are named according the species-specific antigens present on the surface of erythrocytes. These antigens play an important role in inducing immune mediated reactions and can cause complications while transfusing blood. Thus, both the donor and the patient’s blood must be checked carefully before transfusion.
Blood groups observed in the common domestic and pet species are briefly described below:
- DOGS: the blood group system includes DEA 1.1, DEA 1.2, DEA 3, DEA 5, and DEA 7 where DEA 1.1 negative is the universal donor. Here, DEA represents Dog Erythrocyte Antigen. In dogs, the naturally occurring alloantibodies are of lesser clinical significance and if it’s the dog’s first transfusion, a transfusion reaction is not anticipated as the antibodies haven’t formed yet. So basically, dogs can receive their first transfusion safely without being typed or cross matched.
- CATS: There are 3 blood groups reported in cats in ABO blood group system.
- Type A (most common)
- Type B
- Type AB(extremely rare)
There is no universal donor for cats.
As cats have natural alloantibodies, their blood should always be blood typed or cross matched prior to transfusion due to the high possibility of fatal blood transfusion reactions.
Donor Selection
The screening process for blood donors involves a full physical exam by a licensed veterinarian in addition to a complex review of the donor and patient’s health history.
The following conditions must also be checked:-
- Donor’s temperament should be friendly.
- Age should be appropriate.
- There should be no history of blood transfusions or pregnancy.
- The blood should be free from diseases.
Dose Collection
- In general, 2-3 ml/kg of the whole blood will raise the packed cell volume (PCV) by 1%
- The dosage of ANY blood product is 10-30 ml/kg
Site For Collection of Blood For Transfusion
Animal – Site For Collection
- Cats- Jugular
- Dogs- Jugular
Administration rate
- It depends on:
- Anemic status of the animal
- Age of the animal
- Health of the animal
- Blood is administered slowly over first 30 minutes (0.25 ml/kg) and remainder within 1-4 hours.
- In emergency situation such as hemorrhage shock, blood can be administered as rapidly as deemed necessary.
- Blood should never be infused over a period longer than 4 hours.
- Blood must not be given with fluids containing calcium or hypotonic fluid as these can cause the cells to lyse.
Steps of Blood Transfusion
Step 1: Visual inspection of the blood unit (for size, number, expiration date, donor species, blood type, any macroscopic abnormalities indicating contamination and presence of clots)
Step 2: Attaching blood transfusion administration set to the blood unit
Step 3: Connecting it to the patient’s catheter and limiting the infusion rate.
Step 4: Carefully monitoring for physiological parameters and adverse reaction during the transfusion using a Transfusion Monitoring Chart.
Step 5: When the transfusion is complete, flushing the infusion site with 0.9% saline before initiation of other infusions or drugs.
Step 6: Checking PCV 1-6 hours after the transfusion.
Effect of Temperature On Blood Transfusion
- Blood products should be warmed slowly to body temperature before administration to prevent hypothermia and reduce vasoconstriction.
- In urgent situation, the bag is pulled from the refrigerator and is given at a rapid rate but the blood is warmed in the IV line by going through warm water bath.
Complications
- Immune mediated reactions (e.g. hemolytic transfusion reaction, noncardiogenic pulmonary edema.
- Non immune mediated reactions (e.g. sepsis, hemolysis)
- Delayed transfusion reactions
- Infectious disease transfusion
Meet our team
members
#Create
#Animate

Dr. Priya Sharma
Director – Heart
Cardiology
Cardiology

Dr. Priya Sharma
Director – Heart
Cardiology
Cardiology

Dr. Priya Sharma
Director – Heart
Cardiology
Cardiology

Dr. Priya Sharma
Director – Heart
Cardiology
Cardiology






